
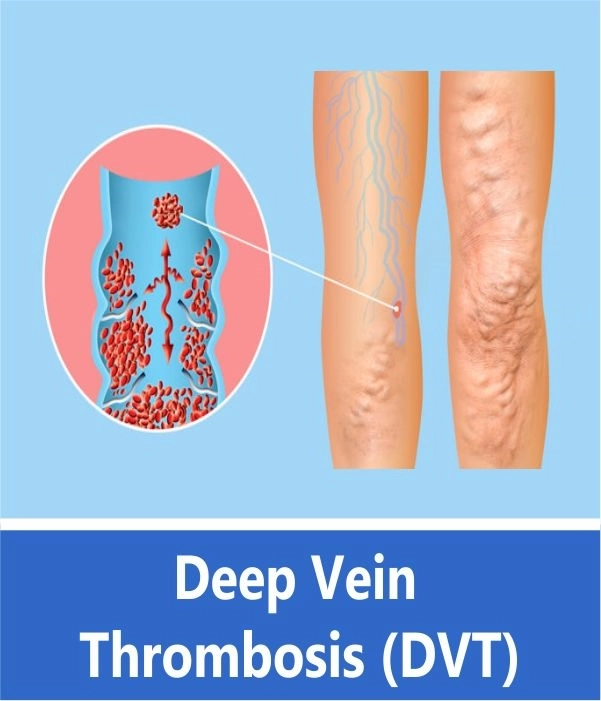
Deep Vein Thrombosis (DVT)

Deep Vein Thrombosis (DVT) is a serious condition that occurs when a blood clot forms in a vein located deep inside your body. A blood clot is a clump of blood that’s turned to a solid-state. In some patients, severe DVT can lead to a clot traveling into the lungs, causing Acute Pulmonary Thromboembolism, which can be fatal. In others, if the DVT persists, it may lead to chronic swelling of the legs, with ulcers and the development of varicose veins.
Deep Vein Thrombosis can develop if you have certain medical conditions that affect how your blood clots. It can also happen if you don’t move for a long time, such as after surgery or an accident, or when you’re confined to bed.
It is now possible to treat severe DVT by means of interventional techniques, by injecting clot-dissolving drugs such as Urokinase directly into the clot. This leads to a rapid decrease in the swelling of the legs, and also prevents pulmonary embolism. In cases where pulmonary embolism has already occurred, or likely, an IVC metal filter can be positioned to prevent further complications.
DVT Symptoms
According to the Centers for Disease Control and Prevention (CDC) Trusted Source, symptoms of DVT only occur in about half of the people who have this condition. Common symptoms include:
- Swelling in your foot, ankle, or leg, usually on one side
- Cramping pain in your affected leg that usually begins in your calf
- Severe, unexplained pain in your foot and ankle
- An area of skin that feels warmer than the skin on the surrounding areas
- The skin over the affected area turning pale or a reddish or bluish color

Blood Clot In Leg Vein
A blood clot in a leg vein may cause pain, warmth, and tenderness in the affected area.
Cases of Patients Treated At Doctor House Cardiovascular Center With DVT
Case 01: Massive Acute DVT Treated by Thrombolysis

A 30-year-old lady presented with a history of Deep vein thrombosis following pregnancy. There was no improvement following conservative treatment with heparin and warfarin. She developed significant changes in the left leg. We cannulated the occluded left iliac vein and infused Urokinase for 24 hours to dissolve the thrombus. Following balloon dilatation was performed, with the restoration of venous flow into IVC. Within 2 weeks, there was good improvement in the edema of the left leg.
Case 02: IVC Filter Placement In Case Of Pulmonary Thrombo Embolism
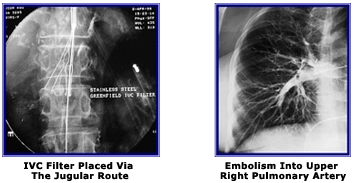
Deep Vein Thrombosis involving the Iliac vein can be complicated by an embolus traveling up to the lungs, and obstructing the Pulmonary artery. The symptoms are chest pain, sudden shortness of breath, drop in arterial saturation. Many cases can be fatal. When a diagnosis of pulmonary embolism secondary to DVT has been made, then it is essential to prevent further episodes. Additionally, if on ultrasound examination, the thrombus in the Iliac vein extends upwards into the IVC or is mobile, it should be prevented from traveling upwards. This can be achieved by placing a metal filter into the IVC, which traps the clot as it travels upwards. Placement of the IVC filter can be achieved percutaneously either from the unaffected side via femoral vein cannulation, or by the jugular vein route. The picture above shows the placement of a filter via the jugular route in a lady who had already had minor episodes of pulmonary embolism.
Case 03: Complete Recanalisation of 6-Month-old Chronic Occlusion of The Left Iliac Vein

An 18-year-old girl developed severe deep vein thrombosis in the left leg. Venous Doppler demonstrated thrombosis involving the deep veins of the entire leg, with total occlusion of the left common iliac vein. She was treated conservatively with heparin and warfarin for three weeks, without any improvement. She continued to have severe swelling of the leg. She was considered an ideal candidate for catheter-directed thrombolysis. In the angiographic laboratory, under local anesthesia, the left superficial femoral vein was entered with an 18 gauge needle, and a 5 French sheath positioned in the vein.
Angiography confirmed that there was total occlusion of the iliac vein, with no flow going upwards into the Inferior Vena Cava. A guidewire was then carefully pushed through the clot and negotiated through the occlusion into the Inferior vena cava. A special infusion catheter was introduced over the wire and an infusion of Urokinase given through this for a period of 24 hours. Check angiography after 24 hours revealed partial flow upwards into the IVC. The entire thrombosed vein was then dilated with an angioplasty balloon, and the final angiogram revealed a fully opened vein with the excellent flow into the Inferior Vena Cava. There was a significant improvement in the swelling, which totally disappeared within 3 days of treatment. Doppler study 10 days after treatment revealed patent common and external iliac veins, with good recanalization seen in the deep femoral and popliteal veins.


